The operational continuity and efficiency of modern surgical environments are fundamentally dependent on the precision of the sterile supply chain. Historically viewed as a peripheral hospital utility, the department responsible for the decontamination and assembly of surgical instruments has undergone a profound semantic and functional transformation into a high-tech logistical hub.1 In contemporary healthcare, several terms describe this centralized center of asset management. The Central Sterile Supply Department (CSSD) remains the most globally ubiquitous designation. Within the DACH region, the formal nomenclature has shifted to the Aufbereitungseinheit für Medizinprodukte (AEMP), reflecting the industrialization of the process.2 As facilities expand to support outpatient surgery centers and external clinics, the term Reprocessing Unit for Medical Devices (RUMED) has gained traction as a more holistic descriptor of the department’s complex supply chain role. In North America, the Sterile Processing Department (SPD) is the standard term, emphasizing the labor-intensive nature of the manual assembly work that advanced technologies now aim to automate.[1]
Regardless of naming conventions, the fundamental objective of these units is the attainment of absolute traceability
Regardless of naming conventions, the fundamental objective of these units is the attainment of absolute traceability and accuracy in instrument assembly.
The integration of advanced tracking technologies is now viewed as the essential mechanism for ensuring that every requested surgical instrument is actually provided to the operating room (OR), eliminating the manual „list-searching“ that historically bottlenecked surgical throughput.
dc c
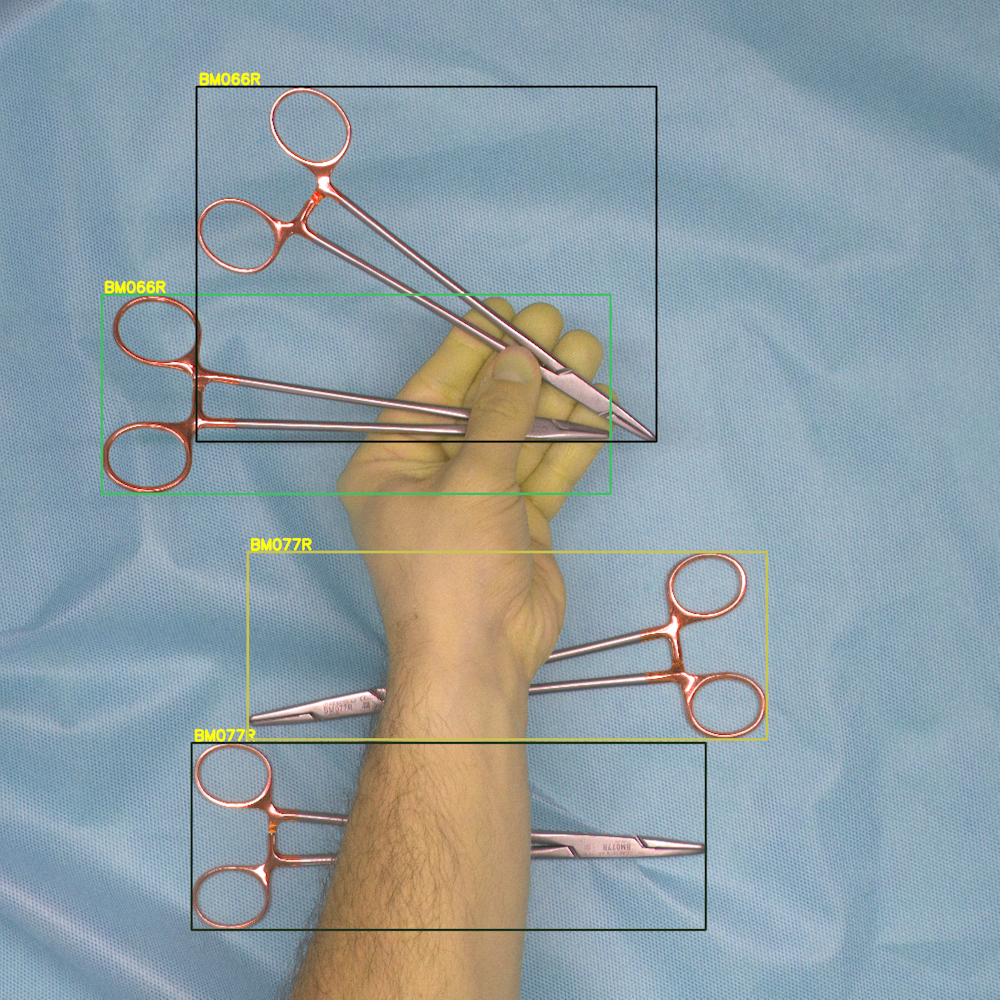
The integration of advanced tracking technologies
Test




